Acute Care
Post-Operative Physiotherapy
Post-operative Physiotherapy discussed on this page will include the immediate post-operative period, but many of the techniques described will be relevant for the entire pre-prosthetic period. Goals of this period are:
- Prevent post-operative respiratory complications
- Assist in wound management
- Prevent complications associated with immobility and amputation surgery (pressure sores, contractures, deconditioning)
- Restore mobility and independence (bed mobility, transfers, crutch / frame / wheelchair mobility)
- Prepare the stump for wearing a prosthesis
- Assist in pain management techniques
- Assist in planning for discharge home or transfer to a rehabilitation setting
Ongoing education forms a large part of these goals.
1. Prevent Post-Operative Respiratory Complications
As well as the effects of an anaesthetic, patients often have pulmonary co-morbidities. Assess and treat as appropriate, including specific respiratory techniques, and early sit out of bed / mobilisation.
2. Assist in Wound Management
Physiotherapy includes:
- Manufacture / fitting of rigid dressings (removeable / non-removeable), and monitoring the fit of the casts over time
- Education of staff / patient on correct donning techniques for removeable rigid dressings, and / or shrinkers and stump bandages, and for signs of incorrect fit / donning
- Monitoring for signs of wound breakdown / infection: temperature spikes that are not explained by infections elsewhere, odours, redness, wound discharges
- Educate the patient:
- Minimise risk of infection
- Protection of the stump in transfers / mobilisation
- Keep dressings dry & intact
- Don't pick at the wound!
- Don't poke objects under the dressings to scratch itches
- Report any changes in pain / odour / temperature
- Do not sit with the stump dangling (which potentially increases dependent oedema and tension on the wound)
3. Prevent Complications Associated with Immobility and Amputation Surgery
Potential complications include pressure areas, contractures, and deconditioning. Techniques to avoid these complications include:
- Instruction / training in bed mobility, transfers, and mobilisation, as appropriate
- Assist and encourage early sit out of bed
- Prescription, and education of positioning programs:
- Prone lying
- Knee extension while lying, sitting out of bed
- No pillows under the knee
- Avoidance of prolonged flexion / abduction / external rotation
- General and /or targeted strengthening / stretching programs
- Cardiovascular program as able or appropriate
4. Restore Mobility and Independence
Please see our pages on Early Mobility
5. Prepare the Stump for Wearing a Prosthesis
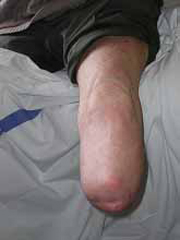
The ideal stump is one that is well-healed, has good vascular supply, soft and mobile scars, minimal pain, minimal oedema, a length sufficient for biomechanical leverage but not too long to restrict choices for prosthetic components, and large surface areas for distribution of pressure. While the surgery plays a large part in creating the ideal stump, Physiotherapy is required to maximise chances of achieving this ideal.
- Oedema reduction
- Rigid dressings
- Fitting and education on use of stump bandaging / shrinkers
- Intermittent Pneumatic Compression Therapy
- Positioning / elevation
- Supply of equipment: legboards
- Education: positioning & massage techniques
- Measurement of changes over time
- Scar management
- Massage / transverse frictions, to mobilise scar tissue and prevent adherent / raised scars
- Education on correct donning of shrinkers, bandages, silicon liners
- Desensitisation
- Massage
- Rubbing, tapping, vibration
- Encouraging normal touch: hands, towels, clothes and sheets
- Range of motion
- Thigh-length rigid dressings
- Splints / backslabs for nights
- Positioning programs and equipment
- Strengthening and range of motion exercises
- Stretching programs
6. Assist in Pain Management Techniques
Please see our pages on Pain Management
7. Assist in Planning for Discharge or Transfer to a Rehabilitation Setting
Active participation with the patient and multidisciplinary team, on negotiating / defining goals to enable discharge or transfer, and using the techniques described to work towards those goals. This may also include training in advanced mobility with crutches for accessing the home, such as car transfers, stairs, ramps, curbs, minimum required endurance.
Links
- EnableNSW, Prosthetic Limb Service, have developed fact sheets on various topics, including caring for your residual limb, caring for your prosthesis, avoiding falls, and managing pain